|
|
Abstract
Dermal scars follow different kinds of injury to the skin including that of the breast. Any lesion on the female breast raises suspicion especially when it mimics breast cancer. Nodular keloidal lesions on the breast may generate some anxiety and scare in the light of public awareness and aggressive preventive campaigns about breast cancer. The psychosocial strain of a false alarm can be severe. Eleven cases of hypertrophic/keloidal lesions of the breast were examined for pattern and extent among female patients presenting at a dermatology clinic who expressed fears about the possibility of underlying disease apart from the scar lesion. None of the cases had any clinical evidence to suggest breast malignancy. Future and larger studies may need to evaluate the anxiety cost of breast cancer scare among black women who develop scars on the breast. Introduction
For women, the breasts represent an important part of the body, especially from the sexual, functional and cosmetic point of view, having also an important emotional and psychological connotation [1]. Breasts have been a symbol of femininity and sexuality since civilization began, so it is not unusual for a woman with any breast lesion to feel that the disease has attacked her body image along with her breast tissue [2]. Women are self-conscious about their breasts and are on the lookout for any suspicious lesions that mimic breast cancer. False alarms are not only psychologically stressful, but they also often force patients to undergo uncomfortable follow-up tests or even surgery, only to discover that they are cancer free. Scars arise after almost every dermal injury including tattoos, superficial scratches and complicate surgery in predisposed individuals. Keloids can develop in any place that an abrasion has occurred as a result of pimples, insect bites, scratching, burns, or other skin trauma. They are more common in some sites such as central chest, the back and shoulders and the ear lobes [3]. Individuals with pigmented skin are more prone to severe skin scarring than white people [3]. Women are more likely to develop heavy scar as are young people under the age of about thirty [4]. There is also a genetic susceptibility to keloids [5]. A scare means sudden mass fear and anxiety over anticipated events or situation: a general state of alarm; a panic: when a subject receives a lot of public attention and worries many people, often unnecessarily [6]. In a situation where "early detection" is emphasized and where new high-tech screening tests are being promoted for breast cancer, it is increasingly possible that everyone with any breast lesion will experience a cancer scare. Studies on how people react when they endure a cancer scare have had mixed results. The psychosocial strain of a false alarm can be severe and may continue after women are declared free from cancer. Many women experience anxiety, worry, despondency, sleeping problems, and negative impact on sexuality and behaviour, and changes in their relationships with family, friends, and acquaintances and in existential values [7,8]. For every cancer survivor, there are several "cancer scare survivors" who are convinced, that they may have cancer when they do not [8]. Can keloidal/hypertrophic scar generate a scare of breast cancer? Keloids are new growths even though benign. Any new lesion on the breast draws attention for clarification. Severe keloidal lesions may be so aggressive that they may be reminiscent of neoplastic disease [9]. Since keloid scars are nodular skin lesions that in severe forms resemble neoplasms, they can cause much physical and mental distress especially when located in sensitive areas like the breasts and nipples [9]. There is a need to highlight breast keloid as a possible avenue for breast cancer scare. Since the breasts are a common site for the keloid prone, there is a need for the caregiver to prioritize how to allay the fears of the affected women.
Case Selection Eleven cases of hypertrophic/keloidal lesions of the breast were examined for the pattern and extent among female patients presenting at a dermatology clinic who expressed fears about the possibility of underlying disease apart from the scar lesion. The pictorial documentation of the different cases was to show the varieties in location and extent among women with breast scars over a time period. The predisposing factors for the emergence of keloidal breast lesions and the body sites affected were identified and documented. None of the patients had any past medical history of breast cancer. A thorough examination of both breasts was carried out by the attending dermatologist with tissue diagnosis where necessary for confirmation. Results
Eleven out of seventy cases (16%); diagnosed with hypertrophic/keloidal scars over a five year period had the breasts affected (Figures 1-11). All eleven cases were female gender. The age range was between 20 to 60years. There was a family history of keloid in eight out of the eleven but no family history of breast cancer. There was no history of breast lump, dimpling, nipple eczema or nipple discharge in any of the patients. Symptoms of the scar lesions included itching, pain, perceived disfigurement and fear of breast cancer. In one case keloidal lesions followed a surgical intervention to remove an initial smaller keloid resulting in the recurrence in a linear fashion along the excision lines and stitches (Figure 9a and 9b). Palpation of both breasts did not reveal any breast lump or significant axillary lymphadenopathy. Five out of the eleven cases had only one breast affected while the remaining had bilateral scar lesions on both breasts. Four of the cases had hypertrophic scars (Figure 1- 4) while the remaining seven had keloidal scars (Figure 5-11). The nipple was the main involvement area in one of the cases with bilateral breast keloidal scar (Figure 6) and it started following a period of breastfeeding. There was anxiety about the exact nature of the scarred lesions in all cases. Skin biopsy confirmed the diagnosis of scar tissue in relevant cases.
 | Fig 1: Early
spontaneous unilateral breast hypertrophic scar. |
|
 | Fig
2: Spontaneous unilateral hypertrophic scar. |
|
 | Fig
3: Post- itch unilateral hypertrophic scar. |
|
 | Fig
4: Under the breast post-candida hypertrophic scar. |
|
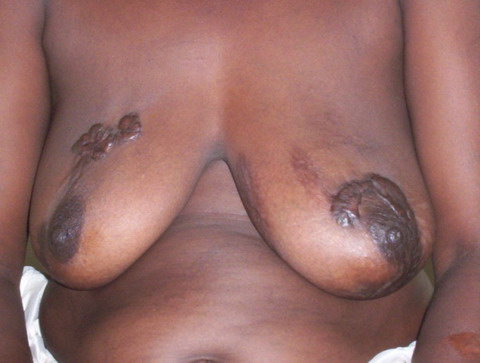 | Fig
5: Bilateral spontaneous breast keloid. |
|
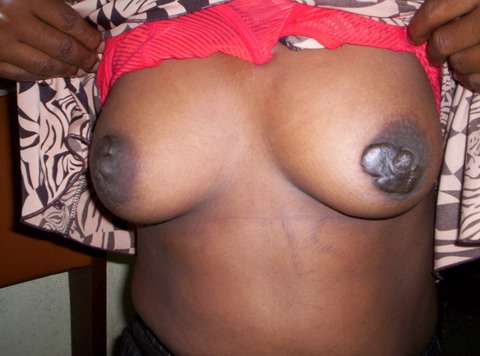 | Fig
7: Post breast feeding bilateral keloid. |
|
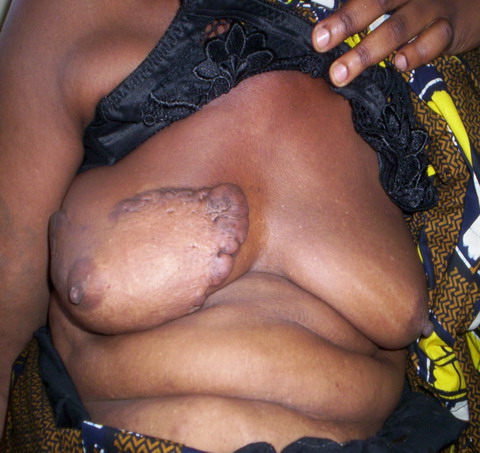 | Fig
8: Unilateral post-traumatic keloid. |
|
|

|
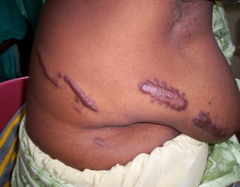
|
| Fig 9: Post-incisional multiple Keloidal scars. |
|
 | Fig
10: breast keloid involving the upper chest wall |
|
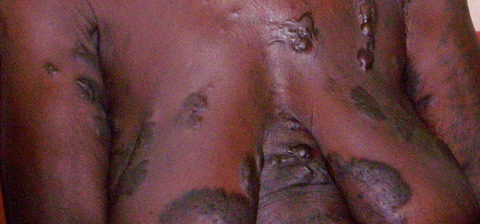 | Fig
11: Spontaneous widespread Keloidal scars. |
|
Discussion
Hypertrophic scars and keloids are common problems, especially in individuals of African descent [3]. Both keloids and hypertrophic scars are characterized by abundant deposition of collagen and glycoprotein. Keloids differ from hypertrophic scars both clinically and histologically. Clinically, keloids extend beyond the original wound, whereas hypertrophic scars remain within the borders of the original wound [10]. Histologically, keloids are composed of disorganized, thick, hyalinized collagen with a prominent mucoid matrix, whereas hypertrophic scars are characterized by fewer, more organized, collagen fibers with a scanty mucoid matrix. The fibroblast concentration has also been reported to be more prominent in hypertrophic scars [11]. Spontaneous Keloidal scars may occur but most follow varieties of trauma from sometimes forgotten or unnoticed insults to the skin. Surgical procedures on the breast including breast augmentation, reduction, therapeutic excision and radiation therapy can result in breast keloids. All causes of primary breast dermatosis may result in scarring on healing in the predisposed individual. In most of the times the underlying injury may not be identifiable. In one study six out of seventy patients with scleroderma exhibited keloidal lesions [12]. Dermatitis artefacta a psycho- dermatological self inflicted wounds affecting the breast in 27 women was reported [13]. The patient usually denies the participation in the injury and there is absence of a rational motive for such process. Hypertrophic/keloidal scars may follow such mutilation of the skin but of the 27 reported cases in the reported series however, none presented clinically with keloidal or hypertrophic lesions of the breast. The clinical presentations included blisters, cigarette burns, excoriations and dermatitis. The author concluded that self-induced dermatitis of the breast is of difficult diagnosis and should be considered when organic disorders have been excluded. This may explain the origin of the primary wounds of some scars whose injury may not have been identifiable. The skin of the breast is subject to both inflammatory and neoplastic process that any skin is subject to. One of the primary goals of diagnosing a breast skin lesion is to rule out a malignant process such as metastatic carcinoma or Paget's disease of the breast, a non-invasive cancer but associated with deeper cancers. Paget's disease of the breast is a malignant condition that outwardly may have the appearance of eczema, with skin changes involving the nipple of the breast. Paget's disease can cause flaky or scaly skin on the nipple, straw-colored or bloody nipple discharge, skin and nipple changes in only one breast or the flattened nipples [14]. Healing of the eczematous nipple may be followed with formation of scars. Unusual keloid-like nodules or scars on the chest that fail to respond to therapy may be primary or metastatic malignancies, and adequate histological verification should be obtained to avoid delay in the proper treatment [15]. Carcinoma en cuirasse was reported to have presented like a keloid in a 63year old woman [15]. It is a form of metastatic cutaneous breast malignancy occurring most commonly on the chest as a recurrence of breast cancer, but it can be the primary presentation. Histologically, the tissue resembles fibrosis with a few tumor cells exhibiting an ''Indian file'' pattern, where the tumor cells forms small lines between collagen bundles. The tumor cells are often overlooked as they appear much like fibroblasts, but with larger, angulated, more deeply basophilic nuclei [15]. The ability to identify cutaneous presentations of breast carcinoma and to obtain histologic verification is critical to avoid delay in proper treatment. A post excisional biopsy scar may occur on the breast producing various degrees of skin thickening, subcutaneous scarring and dystrophic calcification especially if it was infected. This will result in visible changes during radiological investigations and mammography. A surgical scar is an area of fibrosis that is seen on mammogram as an area of architectural distortion or an ill-defined mass mimicking carcinoma. A surgical scar should be located in relative proximity to the incision site. Finding of a post-surgical scar in patients with breast cancer treated with conservation therapy may be suspicious of tumor recurrence. On mammography, a benign surgical scar looks similar to carcinoma. A hypo echoic tract connecting from the mass lesion to the thickened skin at the incision site is helpful in diagnosis of a surgical scar. The atypical may be suspicious enough to cause a scare. It is important for radiologists to be familiar with the spectrum of mammographic abnormalities associated with post biopsy changes and keloidal scars on the breasts [16,17]. Some therapeutic modalities are common to both breast cancer and keloidal scars. The basis for their use in patients with keloidal scars may generate some anxiety in the patient if appropriate counseling is absent. Tamoxifen, a synthetic, nonsteroidal antiestrogen anti breast cancer drug has been shown to inhibit keloid fibroblast proliferation and decrease collagen production [18]. The addition of Tamoxifen may lead to improved wound healing in keloids by decreasing the expression of TGF-b1 [18]. Topical estrogen has been associated with keloid formation. When topical estrogen is applied to normal elderly skin wound margins immediately before wounding and for 24 hours post-wounding it increased the extent of wound heal. The deposition of matrix at day 7 was enhanced in elderly males and females by topical estrogen. Estrogen treatment stimulates matrix deposition [19]. Radiotherapy, also used in treatment of breast cancer, was first introduced as a treatment for keloid scars in 1906 [20]. Keloids remain the commonest type of benign diseases treated by radiotherapy [21]. This can be attributed to the fact that these scars are particularly refractory to most other treatment modalities. Radiation can be used as a monotherapy or combined with surgery to prevent recurrence of keloids following excision. Radiotherapy as monotherapy has been controversial largely due to concerns over post irradiation cancer occurring in some patients [22]. There are only anecdotal reports in the literature of malignancies following treatment of keloids with radiotherapy. Botwood et al report a case of a patient who developed bilateral breast carcinomas 30 years after treatment of chest wall keloids with radiotherapy [23]. Aggressive or morbid keloids, a severe variant of familial keloid is more common in darker skinned individuals than in white subjects, further advocating the genetic component [24]. No single therapeutic modality is best for all keloids. The location, size, and depth of the lesion; the age of the patient; and the past response to treatment determine the type of therapy used. Prevention is key, but therapeutic treatment of hypertrophic scars and keloids includes occlusivee dressings, compression therapy, intralesional corticosteroid injections, cryosurgery, excision, radiation therapy, laser therapy, interferon (IFN) therapy, 5-fluorouracil (5-FU), doxorubicin, bleomycin, verapamil, retinoic acid, imiquimod 5% cream, tamoxifen, tacrolimus, botulinum toxin, and over-the-counter treatments (eg, onion extract; combination of hydrocortisone, silicon, and vitamin E). Other promising therapies include antiangiogenic factors, including vascular endothelial growth factor (VEGF) inhibitors (eg, bevacizumab), phototherapy (photodynamic therapy [PDT], UVA-1 therapy, narrowband UVB therapy), transforming growth factor (TGF)-beta3, tumor necrosis factor (TNF)-alpha inhibitors (etanercept), and recombinant human interleukin (rhIL-10), which are directed at decreasing collagen synthesis [25].
Conclusion
Keloid is both physically and emotionally stressful for the patient and worse still when it involves a sensitive part of the body that defines feminity. Breast lesions including hypertrophic/keloidal scars may mimic cancer of the breast and cause a scare.. Future studies may need to evaluate the anxiety cost of breast cancer scare among black women who develop scars on their breasts. References
1. Whitaker-Worth DL, Carlone V, Susser WS et al. Dermatologic diseases of the breast and nipple. J Am Acad Dermatol 2000; 43: 731-751.
2. Miguel Sabino Neto, Maria Fernanda Demattê, Marcia Freire, Élvio Bueno
Garcia, Marina Quaresma, Lydia M. Ferreira. Self-Esteem and Functional
Capacity Outcomes Following Reduction Mammaplasty. Aesthetic Surgery Journal
2008 Volume 28(4) July/August 417-420.
3. Oluwasanmi JO. Keloids in the African. Clin Plast Surg. 1974; 1:179-95.
4. Kelly AP: Medical and surgical therapies for keloids. Dermatol Ther 2004, 17:212-8
5. Marneros AG, Norris JE, Olsen BR, Ernst Reichenberger: Clinical genetics of familial keloids. Arch Dermatol 2001, 137:1429-34
6. Dictionaries online: Cambridge Advanced Learner's Dictionary. Cambridge University Press 2010. http://dictionary.cambridge.org/dictionary/british/scare_2
7. Brodersen J, Thorsen H, Kreiner S. Validation of a condition-specific measure for women having an abnormal screening mammography. Value in Health 2007;10:294-304
8. Brodersen J. Measuring psychosocial consequences of false-positive screening results - breast cancer as an example. Department of General Practice, University of Copenhagen. 2006. http://cms.ku.dk/sund-sites/ifsv-sites/ifsv-inst/ominstituttet/afdelinger/almen_medicin/medarbejdere/publicationdetail/?id=1109837.
9. Ardeshir Bayat, Guyan Arscott, William E R Ollier, Mark W J Ferguson , D Angus McGrouther : Aggressive keloid': a severe variant of familial keloid scarring: J R Soc Med 2003;96:554-555
10. Berman B, Zell D, Perez OA. Keloid and hypertrophic scar. WebMD emedicine 2007 Feb 1. Available: www.emedicine.com/DERM/topic205.htm
11. Blackburn WR, Cosman B. Histologic basis of keloid and hypertrophic scar differentiation. Arch Pathol 1966;82:65-71.
12. Adrienne Rencic, Nooshin Ketabchi Brinster, Carlos H Nousari. Keloid Morphea and nodular scleroderma: Two distinct clinical variants of Scleroderma? J Cutan Med Surg 2003; 20-24.
13. A Rodrı´guez-Pichardo,MV Hoffner, B Garcı´a-Bravo,FM Camacho; Dermatitis
artefacta of the breast: a retrospective analysis of 27 patients
(1976–2006): JEADV 2010, 24, 270–274.
14. Alper Parlakgumus, Sedat Yildirim, Filiz Aka Bolat, Kenan Caliskan, Ali Ezer, Tamer Colakoglu, Gokhan Moray: Dermatosis of the nipple: J Can Chir, Vol. 52, No 2, avril 2009; 160-161
15. Kimberly Mullinax, Jack B Cohen, DO Carcinoma En Cuirasse Presenting as Keloids of the Chest: Dermatol Surg 2004;30: 226-228
16. Kimberly B Stigers, Joseph G Kings, Diane D Davey, Carol B Stelling. Abnormalities of Breast caused by Biopsy: Spectrum of Mammographic Findings. AJR 156: 287-291 Feb 1991
17. Pojchamarnwiputh S, Muttarak M, Na-ChiangMai W, Chaiwun B. Benign breast lesions mimicking carcinoma at mammography. Singapore Med J 2007; 48(10) : 958
18. Anthony A. Mikulec, MD; Matthew M. Hanasono, MD; Joanne Lum, BS;James M. Kadleck; Magdalena Kita; R. James Koch, MD, MS. Effect of Tamoxifen on Transforming Growth Factor B1 Production by Keloid and Fetal Fibroblasts. Arch Facial Plast Surg. 2001;3:111-114.
19. Gillian S. Ashcroft, Teresa Greenwell-Wild, Michael A. Horan, Sharon M. Wahl, Mark W. J. Ferguson. Topical Estrogen Accelerates Cutaneous Wound Healing in Aged Humans Associated with an Altered Inflammatory Response. Am J Path.155(4), Oct 1999; 1137-1146.
20. De Bearman R, Gourgerot H: Cheloides des maqueuses. Ann Dermatol Syphilol (Paris) 1906, 7:151.
21. Botwood N, Lewanski , Lowdell C: The risks of treating keloids with radiotherapy. Br J Radiol 1999 , 72:1222-24.
22. Norris JE: Superficial X-ray therapy in keloid management: a retrospective study of 24 cases and literature review. Plast. Reconstr. Surg. (1995) 95(6):1051-1055.
23. Botwood N, Lewanski C, Lowdell C. The risks of treating keloids with radiotherapy. Br J Radiol. 1999 Dec;72(864):1222-4.
24. Bayat A, Arscott G, Ollier WE et al. 'Aggressive keloid': a severe variant of familial keloid scarring. J R Soc Med 2003; 96:554-5
25. Berman B, Valins W, Amini S and Viera MH. Keloid and Hypertrophic Scar. http://emedicine.medscape.com/article/1057599-print [Updated: May 14, 2010]© 2010 Egyptian Dermatology Online Journal |












