|
|
Abstract
A six year old female child with generalized hyperpigmented hyperkeratotic
verrucous plaques with nail and dental abnormalities suggestive of ichthyosis
hystrix type of epidermal nevus is being reported in view of the rarity
of this condition.
Introduction
The term systematized epidermal nevus is used for lesions that are bilateral
and excessive and the similarity to the lesions of ichthyosis is emphasized
in the term ichthyosis hystrix. The term ichthyosis hystrix is used to describe
several rare skin disorders in the ichthyosis family of skin disorders characterized
by massive hyperkeratosis with an appearance like spiny scales. This term
is also used to refer to a type of epidermal nevi with extensive bilateral
distribution [1].
Patients with extensive epidermal nevi or those with epidermal nevi and
systemic abnormalities should be suspected of having the epidermal nevus
syndrome [1]. An estimated one third of
individuals with epidermal nevi have involvement of other organ systems;
hence, this condition is considered to be an epidermal nevus syndrome (ENS).
Case Report
A six year old girl child presented to the outpatient department of Dermatology,
STD and Leprosy SMHS hospital (associated teaching hospital of Government
Medical College Srinagar) with history of multiple warty lesions all over
the body. Her mother reported that the child was a product of full term,
normal vaginal delivery, delivered at home with no history of consanguinity
and with normal developmental milestones. When the child was about two months
of age, parents noticed small, skin coloured, velvety lesions on her right
middle finger. Gradually, over years the lesions became darker and more
warty and spread to involve other digits of right hand, and then other limbs
and trunk. The lesions were not associated with pruritus, blister formation
or secondary infection. No relevant history of seizures, mental retardation,
headache, arthralgias, visual or hearing abnormalities were found. None
of her siblings or parents had history of any skin disease. Drug history
of mother during pregnancy was not significant.
General physical examination and systemic examination were within normal
limits.
On cutaneous examination bilateral, more or less symmetrical, linear
[along the lines of Blaschko], hyperpigmented, hyperkeratotic, verrucous plaques
were found over the dorsa of fingers extending to the dorsal surface of
hand with greater involvement of right side than left (fig 1, 2).
Both dorsal and plantar surface of feet were involved in a related but less
severe fashion (fig 3). Isolated hyperpigmented, hyperkeratotic papules
were noticed in a linear pattern over extremities more over the extensor
surface. Similar papules were present over ear lobes, neck, and umbilicus
and on trunk along axillae and groins (fig 4). Scalp, face and palms
were spared. Finger nails of the involved digits were dystrophied. Dental
abnormalities in the form of enamel hypoplasia were seen on central and
lateral incisors of upper jaw while hair and mucosa were normal.
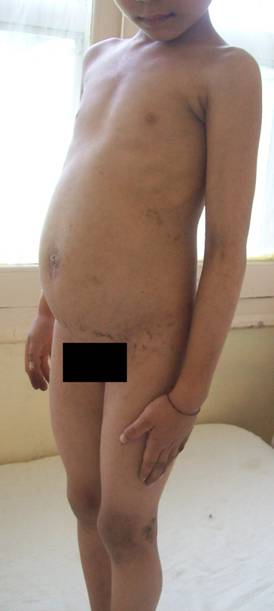 | Fig 1:
Generalised Hyperpigmented, verrucous plaques and papules
particularly around the umbilicus. |
|
 | Fig
2: Linear (along Blashcko's lines) verrucous plaques over
dorsa of fingers. |
|
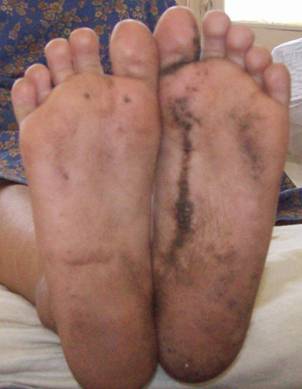 | Fig
3: Linear hyperpigmented, hyperkeratotic plaques over
planter surface of feet. |
|
 | Fig
4: Linear skin coloured papules and plaques over inner
aspect of upper arms. |
|
Detailed neurological, opthalmological, otolaryngological and orthopedic
consultations were sought and revealed no abnormalities.
Routine investigations on blood and urine were within normal limits.
Calcium and phosphorus levels were normal.
Ultrasonographic examination of abdomen was also normal. Skeletal survey
in form of X-rays did not reveal any abnormalities.
Histo-pathological examination of a representative lesion revealed acanthosis,
papillomatosis and hyperkeratosis of epidermis.
On the above constellation of clinical features (history, typical morphology
and generalized, roughly bilaterally symmetrical involvement) a diagnosis
of ichthyosis hystrix type of epidermal nevi (systematized epidermal nevus)
was made.
Discussion
Epidermal nevi arise from the embryonic ectoderm, which differentiates
not only into keratinocytes but also into cells forming the epidermal appendages,
therefore these nevi are best classified according to their predominant
component into keratinocytic (non-organoid) nevi and organoid nevi such
as sebaceous, follicular, and sweat gland nevi.[2]
Keratinocytic (non-organoid) nevi are also known as nevus verrucosus
and verrucous epidermal nevus. These nevi occur mainly on the trunk and
limbs, although occasionally the head is involved, particularly as part
of a very extensive lesion. They may be congenital but in over 50% of cases
the onset is after birth, usually in the first year of life but occasionally
as late as adolescence.
The term systematized epidermal nevus is used for lesions that are bilateral
and excessive and the similarity to the lesions of ichthyosis is emphasized
in the term ichthyosis hystrix [2].
Ichthyosis hystrix is a descriptive term for a heterogenous group of
skin conditions characterized by massive, spiky and warty accumulations
of hyperkeratosis. In 1954, Curth and Macklin[3]
described a family affected to varying degrees with palmoplantar keratoderma
and symmetric involvement of dark, verrucous hyperkeratosis, a disorder
now called as ichthyosis hystrix of Curth & Macklin. It is an autosomal
dominant disorder that clinically resembles epidermolytic hyperkeratosis.
Clinical expression varies, even within families, from palmoplantar keratoderma
to a severe, generalized involvement. There can be widespread, patchy, thick,
grey-brown hyperkeratosis, most marked on extensor surface of arms and legs.
Patients with extensive involvement resemble those with severe epidermolytic
hyperkeratosis without palmar/plantar involvement with verrucous or porcupine-like
(hystrix) hyperkerkeratosis. However, in contrast to epidermolytic hyperkeratosis,
blistering does not occur. Histological examination of the epidermis shows
acanthosis, papillomatosis, and severe orthokeratotic hyperkeratosis, with
frequent binucleate cells [4]. Study of
three generation family with ichthyosis of Curth and Macklin identified
a mutation in the variable tail domain (V2) of the keratin -1 gene [5].
Patients with extensive epidermal nevi or those with epidermal nevi and
systemic abnormalities should be suspected of having the epidermal nevus
syndrome (ENS). Epidermal nevus syndrome has been synonymously linked with
Schimmelpenning syndrome, Feurstein-Mims syndrome, and Solomon syndrome
[1].
Epidermal nevus syndrome affects men and women equally and presents within
the first 40 years of life. Inheritance is mostly sporadic. Although the
exact incidence of epidermal nevus syndrome is unknown, a study of 119 cases
of epidermal nevus syndrome showed that 33% of patients showed two or more
abnormalities, 16% showed two or more abnormalities, 10% showed three or
more abnormalities and 5% showed five or more abnormalities [1].
Solomon and Esterly [6] provided a detailed
account of the spectrum of epidermal nevi seen in the epidermal nevus syndrome.
They described seven types of lesions. The majority of patients had nevus
unius lateralis; 20 percent of patients had ichthyosis hystrix.
Mucocutaneous changes other than epidermal nevus which may be associated
with ENS are haemangiomas and pigmentary changes found in 10 to 20 percent
of patients [7]. Less common findings are
hair abnormalities, dental abnormalities, and dermatomegaly; various cutaneous
tumors may develop within the epidermal nevus.
A wide range of skeletal abnormalities has been reported [7,8,9].
The incidence of skeletal changes has ranged from 15 percent to 70 percent.
Neurologic abnormalities occur in 15 percent to 50 percent of cases. 9 to
30 percent of patients with epidermal nevus syndrome have ocular abnormalities
[10].
The major treatment consists of symptomatic therapy of the complications
and for cosmetic purposes. The various modalities involve excision of small
nevi, while treatment of the larger and facial nevi involves application
of topical preparations, cryotherapy, electrodessication, dermabrasion,
curettage and skin grafting.
A diagnosis of epidermal nevus syndrome should be thought in patients
with extensive epidermal nevi and or systemic abnormalities. A thorough
muco-cutaneous, neurologic, ophthalmic and orthopaedic examination is necessary
with specific investigations depending on the involved system.
References
1. Duncan KO, Geisse JK, Leffel DJ. Benign epithelial tumours.
In: Epidermal and appendageal tumours. In: Fitzpatrick's dermatology in
general medicine. 7th edn. Eds. Wolff K, Goldsmith LA, Katz S, Gilchrest
BA, Paller AS, Leffell DJ. McGraw-Hil Division, NY, 2008:1060-61.
2. Rogers M. In: Epidermal naevi / epidermal naevus syndromes.
In: Textbook of Pediatric Dermatology. 2nd edn. Eds. Harper J, Oranje A,
Prose N. Blackwell Publishing Ltd., 2006: 1125.
3. Curth HO, Macklin MT. The genetic basis of various types
of ichthyosis in a family group. Am J Hum Genet 1954; 6: 371-82.
4. Fleckman P, Digiovanna JJ. The Ichthyoses. In: Disorders
of epidermal differentiation and keratinization. In: Fitzpatrick's dermatology
in general medicine. 7th edn. Eds. Wolff K, Goldsmith LA, Katz S, Gilchrest
BA, Paller AS, Leffell DJ. McGraw-Hil Division, NY, 2008: 414
5. Sprecher E, Ishida-Yamamoto A, Becker OM, Marekov L,
Miller CJ, Steinert PM, Neldner K, Richard G (2001) Evidence for novel functions
of the keratin tail emerging from a mutation causing ichthyosis hystrix.
J Invest Dermatol 1164:511-519
6. Solomon LM, Esterly NB: Epidermal and other congenital
organoid nevi. Curr Probl Pediatr 1975; 6:1-56
7. Eichler C et al: Epidermal nevus syndrome: Case report
and review of clinical manifestations. Pediatr Dermatol 6:316, 1989.
8. Happle R: Epidermal nevus syndromes. Semin Dermatol 1995;
14: 111- 121
9. Chow MJ, Fretzin DF: Epidermal nevus syndrome: Report
of association with chondroblastoma of bone. Pediatr Dermatol 1989; 6: 358.
10. Mansour AM , Barber JC, Reinecke RD, Wang FM: Ocular
choristomas. Surv Ophthalmol 33:339-58, 1989.
© 2011 Egyptian Dermatology Online Journal
|




