|
|
Abstract
Acute febrile neutrophilic dermatosis or Sweet's syndrome is the most
common neutrophilic dermatoses, a nosological framework of a widening
spectrum of anatomical and clinical entities and a new set of atypical,
unusual or complex forms. This syndrome is often associated with
hematologic malignancies. Other non-neoplastic associations have been,
however, described. We report a case of a patient in whom the onset of
Sweet's syndrome has led to the diagnosis of lymph node tuberculosis.
The occurrence of Sweet's syndrome must perform a complete assessment
including a search of tuberculosis.
Introduction
Sweet's syndrome is characterized by pyrexia, elevated neutrophil
count, tender erythematous skin lesions (papules, nodules and plaques)
and a diffuse infiltrate consisting predominantly of mature neutrophils
typically located in the upper dermis. The classical form is preceded by
an upper respiratory tract infection or gastrointestinal tract
infection. The diagnostic criteria are clinical, biochemical and
histological. This syndrome is often associated with hematologic
malignancies and even infections such as tuberculosis [1].
We report a case of Sweet's syndrome revealing lymph node tuberculosis.
Case Report
A 32-year-old woman, without previous history of drug administration,
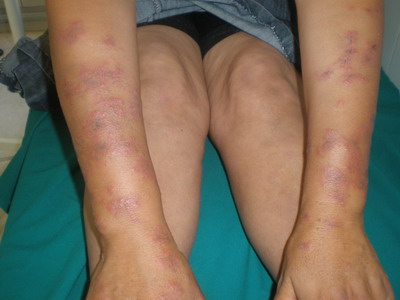
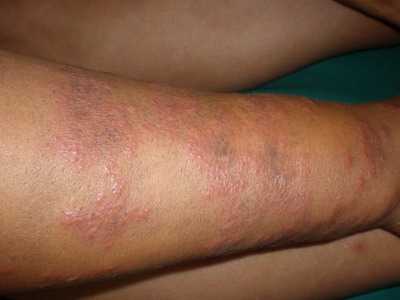
was admitted to the hospital because of a-week history of dermal
erythematous plaques on the limbs and chest (Fig 1, 2, 3)
associated to arthralgias.
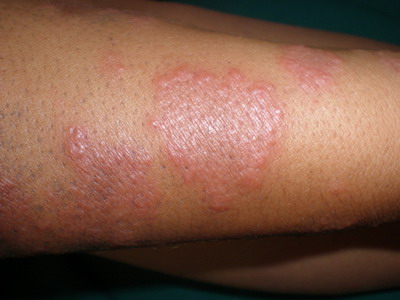 |
Fig 1, 2 and 3: Extensive and infiltrated maculopapular erythema on
the limbs. |
|
Physical examination revealed conjunctival hyperemia, fever 38 ° C
and right cervical sub-maxillary angle lymphadenopathy, fixed at 3 cm of
diameter. The ultrasound examination showed cervical lymph nodes under
the right digastric muscle. Chest x-ray was normal.
The lymph node biopsy has been in favor of tuberculosis.
There was a high sedimentation rate to 85 at the first hour, white
blood cells to 6300 elements per mm³. The remaining balance was normal.
On histologic examination (Fig4), the dermis is edematous, has
an inflammatory infiltrate, made of numerous polymorphonuclear
neutrophils with few evidence of leucocytoclastic vasculitis, and
associated with mononuclear cells. It has not been observed histological
signs of malignancy. The diagnosis of Sweet syndrome associated with
lymph node tuberculosis was established. The patient was treated with
colchicine at a dose of 1mg/kg/jour. All skin lesions resolved rapidly.
An anti-tuberculosis treatment was also instituted.
 |
Fig 4: Inflammatory infiltrate of the dermis, made of
numerous polymorphonuclear neutrophils without vasculitis |
|
Discussion
Described in 1964 by Sweet, this syndrome is characterized by the
sudden influx of neutrophils into the dermis in the absence of any
infection [2]. The same infiltration by
neutrophils may occur in deep organs [3].
It is usually observed in adults in the fourth decade and more often in
women than in men [4]. Childhood cases
are rare. In about 75% of cases the rash is preceded by signs of
rhinitis, pharyngitis, cough, malaise, muscle pain or digestive
problems, all suggestive of a viral infection. The skin lesions then
appear suddenly are in the form of erythematous papules and nodules.
Plaques are very limited, painful, with raised hummocky surface
extending centrifugally, leaving a central depression. These plates may
have a vesicular or pustular surface. They are limited or sometimes even
multiple and disseminated. The lesions are first asymmetric in
distribution then they become symmetrical. They sit preferentially in
the face, neck, the posterior surface of the forearms, backs of hands
and fingers, lower limbs and rarely on the back [5].
The diagnosis usually poses few problems. The clinical appearance of
lesions, their distribution and massive infiltration of the dermis by
neutrophils without vasculitis are the major criteria of diagnosis [6].
In our patient, the absence of leukocytosis and the presence of
cervical lymph nodes, led us to push the exploration that confirmed the
diagnosis of tuberculosis. Our observation stresses the importance of a
comprehensive assessment (chest radiograph, Mantoux test and research of
Koch bacillus) before any suspicion of tuberculosis, especially in
endemic countries like ours.
SS is most often idiopathic, but sometimes associated with various
pathological conditions including malignancies. It is sometimes
associated with visceral cancers such as testicular carcinoma and
ovarian carcinoma. It has also been described in association with some
infectious diseases such as tuberculosis, toxoplasmosis, salmonellosis,
or infection with HIV [7].
In the series of Boudghene-Stambouli and al [8],
the SS was significantly associated with chronic lymphocytic leukemia
complicated by tuberculous ascites, lymph node tuberculosis and ulcer
perianal tuberculosis.
The pathogenesis of SS remains unknown. Some authors suggest that
lesions may be secondary to a hypersensitivity reaction to an allergen [9].
Interleukin-1 might play a role as mediator of inflammation [10].
The GCSF (granulocyte colony stimulating factor), growth of neutrophils,
is certainly also involved, either by increasing its synthesis or by the
existence of hypersensitivity to this cytokine [11].
It could finally be a genetic predisposition. Moreover SS seems more
common in Japan, and HLA-Bw54 has been described as a risk factor [12].
Treatment is symptomatic. Efficiency of systemic corticosteroids is
spectacular [5].
If SS was associated to tuberculosis, other therapies such as
colchicine may be used [8,13].
Conclusion
Sweet's syndrome is not uncommon. It is most often idiopathic, but
sometimes associated with other diseases, especially infection. The
association with tuberculosis should be noted. Corticosteroids should be
handled with great caution. Treatment by colchicine must be useful,
because of its efficiency.
References
1. Von den Driesch P. Sweet's syndrome (acute febrile
neutrophilic dermatosis). J Am Acad Dermatol 1994;31:535-56.
2. Sweet RD. An acute febrile neutrophilic dermatosis.
Br J Dermatol, 1964; 76: 349-356.
3. WALLACH D. Les dermatoses neutrophiliques. Presse
Méd. 1991; 20: 105-107.
4. Sweet RD. Acute febrile neutrophilic dermatosis. Br J
Dermatol, 1979; 100: 93-9.
5. Samon-Ehr V, Estève E, Serpier H et al. Dermatose
neutrophilique aigue fébrile pustuleuse et bulleuse révélant une
leucémie aigue myéloblastique. Rev Méd Interne 1995; 16: 347-350.
6. Su WPD, Liu HNH. Diagnostic criteria for Sweet's
syndrome. Cutis 1986; 37: 167-74.
7. Von den Driesch P. Sweet's syndrome (acute febrile
neutrophilic dermatosis). J Am Acad Dermatosis). J Am Acad Dermatol
1994; 31: 535-56.
8. Boudghene -Stambouli O, Merad-Boudia A. Dermatose
aigue febrile neutrophilique aspect clinique, évolutif et thérapeutique.
A propos de 55 observations. Les nouvelles dermatologiques 1996; 15:
702-706.
9. Petrozzi JW, Warthan TL. Sweet's syndrome: unique
local response to streptococcal antigen. Cutis 1976; 17: 267-72.
10. Going JJ. Is the pathogenesis of Sweet's syndrome
mediated by interleukin-1? Br J Dermatol 1987; 116: 282-3.
11. Park JW, Mehrotra B, Barnett BO, Baron AD, Venook
AP. The Sweet syndrome during therapy with granulocyte
colony-stimulating factor. Ann Intern Med 1992; 116: 996-8.
12. Mizoguchi M, Matsuki K, Mochizuki M et al. Human
leukocyte antigen in Sweet's syndrome and its relationship to Behçet's
disease. Arch Dermatol 1988; 124: 1069-73.
13. Suehisa S, Tagami H, Inoue F, Matsumoto K,
Yoshikuni K. Colchicine in the treatment of acute febrile neutrophilic
dermatosis (Sweet's syndrome). Br J Dermatol 1983; 108: 99-101.
© 2011 Egyptian Dermatology Online Journal
|