|
|
Abstract
Impetigo herpetiformis (IH) is a rare pustular form of psoriasis in pregnancy,
associated with constitutional symptoms and complications of secondary infection
and sepsis and an increased risk of fetal abnormalities and stillbirths.
Here we present a series of four cases of impetigo herpetiformis, primarily
treated with systemic corticosteroids. Dapsone and cyclosporin were added
in patients with persistence of skin lesions or showing resistance to steroids.
Lesions resolved in all with good obstetric outcome, except in one who had
an intrauterine death (IUD) at 34 weeks of gestation despite good response
of skin lesions to steroids, providing additional evidence that IH is associated
with placental insufficiency, stillbirths and neonatal deaths. In this article
we emphasize the importance of early diagnosis and treatment to minimize
maternal and fetal mortality and morbidity and considering other therapeutic
options like dapsone and cyclosporine as alternative treatment options for
IH in case of poor response to corticosteroids.
Introduction
Impetigo herpetiformis is a rare, life threatening pustular dermatoses
of pregnancy with an obscure etiology. First described by Hebra in 1872
[1], this disorder is characterized by erythematous
plaques with grouped sterile pustules at their margins, starting as symmetrical
lesions in intertrigenous areas that extend centrifugally, associated with
severe constitutional symptoms. It usually starts in the last trimester,
but may occur as early as third month of the pregnancy. Mucous membranes
and nails can also be affected. Hypocalcemia is commonly associated with
IH. The disease resolves promptly postpartum. The main complications are
those of placental insufficiency, an increased risk of still births, fetal
abnormalities and neonatal deaths. We present a series of four cases of
impetigo herpetiformis, all presenting in the second and third trimester
of pregnancy.
Case Reports
Case 1:- A 22 year old primigravida, presented at 24 weeks of
gestation, with history of generalized pustular eruption for two weeks.
Dermatological examination revealed erythematous plaques studded with minute
grouped pustules coalescing to form bigger sheets of lesions, distributed
over the neck, trunk, arms, dorsum of hands, legs and buttocks (Fig 1).
Oral cavity examination revealed geographic tongue.
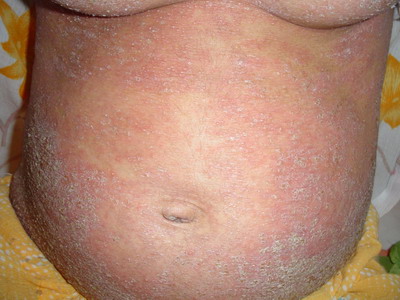
| Fig 1: Impetigo herpetiformis in a 22
year old female. There are multiple ill-defined
erythematous scaly plaques with dried up pustules on
the abdomen and infra-mammary folds. |
|
Case 2:- A 27 years old primigravida, presented with fever and
generalized pustular lesions at 26 weeks of gestation for two weeks. On
examination, erythematous plaques with an active polycyclic elevated border
comprised of micropustules were distributed on the face, neck, trunk and
extremities (Fig 2). Mucosae were normal.

| Fig 2: Impetigo herpetiformis in a 27
year old female showing multiple erythematous
plaques many of which have peripheral rim of
desiccated pustules. |
|
Case 3:-A 29 years old multigravida, a known case of psoriasis
for 7 years, presented at 28 weeks of gestation, with multiple plaque type
lesions, studded with pustules for three weeks. The lesions initially appeared
over the submammary region that rapidly progressed to involve chest, lower
abdomen and limbs (Fig 3). Her earlier pregnancy was uneventful.
On examination, pinpoint pustules over an erythematous background were present.
Mucosae were normal.
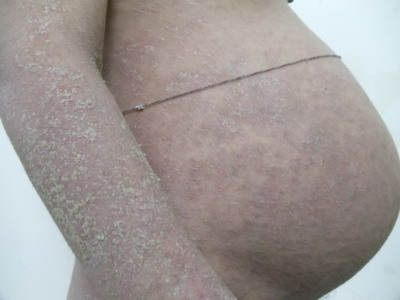
| Fig 3: Impetigo herpetiformis in a 29
years old multigravida showing diffuse silvery white
scaling which has occurred due to drying and
desiccation of pustules under a background of dull
erythema. |
|
Case 4:- A 21 years old primigravida presented at 28 weeks of
gestation, with widespread painful erythematous rash with pustules for the
last one month. Dermatological examination revealed widespread erythemato-squamous
plaques with tiny superficial pustules. (Fig 4). Geographic tongue
with fissures was also present.
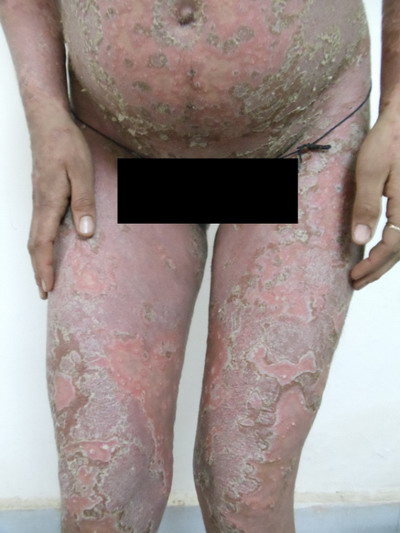 |
Fig.4a : Impetigo herpetiformis in a 21 year old
primigravida showing widespread scaly erythematous plaques with
tiny superficial pustules in frontal view |
|
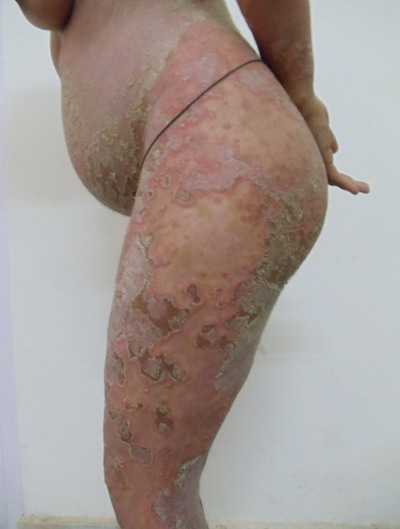 |
Fig.4 b: Impetigo herpetiformis in a 21 year old primigravida showing
widespread scaly erythematous plaques with tiny superficial pustules in
lateral view |
|
The lesions were associated with an intense itching and burning sensation
and severe constitutional symptoms in all cases. Personal history of psoriasis
was present in one patient (case 3), but there was no family history of
psoriasis. Systemic and obstetrical examinations were normal.
Laboratory findings revealed leucocytosis and raised ESR in all patients.
Liver function tests and renal function tests were within normal limits.
Serum calcium level was low in one patient (case 1). Gram stained smear
of pustules was negative and culture from the pustules was sterile in all
the cases. Histopathology of skin was consistent with pustular psoriasis
in all cases. Ultrasonography did not reveal any abnormalities except intrauterine
growth retardation in one patient (case 3). Based on typical clinical features
and histopathological findings, patients were diagnosed to have impetigo
herpetiformis.
In cases 1 and 2, systemic steroids at a dose of 60 mg / day, along with
other supportive measures were started. The lesions started regressing within
two to three weeks. Dapsone 100 mg/day was added and dose of steroids tapered
slowly to a minimum of 10mg/day. The treatment was continued throughout
the pregnancy and stopped within few days after delivery.
In case 3, systemic steroids at a dose of 60mg/day were started. Her
symptoms were adequately controlled in 2 to 3 weeks. Tapering of steroids
was started and the eruption remained stable thereafter. She went into spontaneous
labour at 34 weeks, delivering a dead baby prematurely. Steroids were further
tapered and stopped.
In case 4, systemic steroids at an initial dose of 60 mg /day for 3 weeks
failed to control the disease. Cyclosporine at a dose of 4mg/kg body weight
was added in two divided doses. The skin lesions started regressing within
1 to 2 weeks. The corticosteroid dose was tapered gradually to 10 mg/day
and along with cyclosporine at 100mg/day were continued, with strict monitoring
of all relevant parameters, till delivery at thirty-eight weeks and stopped
thereafter.
Discussion
There is a considerable debate surrounding the classification of IH.
Hebra [1] classified it as specific dermatoses
of pregnancy. Some consider it to be an acute phase of generalized pustular
psoriasis precipitated by endocrine changes of pregnancy in individuals
with subclinical disease [2,3]
whereas others describe it as an entity distinct from psoriasis [4].
The pathogenesis of this disease remains unclear but is attributed to
high levels of progesterone during the last trimester of pregnancy, low
levels of calcium and reduced levels of epidermal skin-derived antileukoproteinase
activity [5].
The onset in our patients was between 24 to 26 weeks of gestation as
reported earlier [6,7].
Geographic tongue was present in two of our patients, consistent with earlier
reports [2]. Cases of IH with hypoparathyroidism
have been reported where authors speculated that the patients with latent
hypoparathyroidism may become hypocalcemic because of increased demand for
calcium in the last trimester of pregnancy [8].
Family history was found in none of our patients, comparable to the findings
of Ott et al. [6] but has been reported
at other places [9].
Oral corticosteroids are the mainstay of treatment in IH [7].
Two of our patients were treated with dapsone after an initial response
to oral corticosteroids. Use of dapsone may be considered in subacute and
chronic forms of generalized pustular psoriasis, and may be valuable in
atypical variants [10]. It was found to
be effective, without any adverse effect to both mother and fetus. In one
patient (case 3), marked improvement was seen in skin lesions with steroids
but went into spontaneous labour that culminated into an IUD. IH occurring
during nine successive pregnancies, with eight fetal deaths has been reported
[9]. Of late, cyclosporine as well as methotrexate
has been used in IH [11,12].
Cyclosporin has been administered in patients with IH and in most of cases,
not as a monotherapy but in combination with low dose systemic corticosteroids.
In one of our patients (case 4), unresponsive to steroids, cyclosporine
was added, that helped to achieve control of the disease, as has been reported
earlier also [13]. Despite placental transfer,
cyclosporine seems to be rather safe. Children exposed in utero to cyclosporine
have been shown to have normal renal function. Use of the lowest active
dose and careful monitoring of the fetus is advisable [14].
Conclusion
IH is associated with placental insufficiency posing an increased risk
to the fetus. The awareness and recognition of the clinical presentation
and careful management is important. Alternative therapeutic options in
the form of dapsone or cyclosporine may be considered, when corticosteroids
are not enough to control the eruption alone or as a steroid-sparing agent.
In any case, total regression of lesions must be expected after delivery.
References
1. Hebra F. Ueber einzelne wahrend Schwangerschaft, des
Wacherbette unde bei uterinal. Krankheiten der Frauen zu beobachtende Hautkraukheiten.
Wien Med Wochenschr. 1872; 48: 1197-1202.
2. Sauer GC, Geha BJ. Impetigo herpetiformis: Report of
a case treated with corticosteroid - review of literature. Arch Dermatol
1961; 83: 119-126.
3. Baker H, Ryan TJ. Systemic corticosteroids and folic
acid antagonists in the treatment of generalized pustular psoriasis. Br
J Dermatol 1969; 81: 134-45.
4. Lotem M, Katzenelson V, Rotem A, Hod M, Sandbank M. Impetigo
herpetiformis : a variant of pustular psoriasis or a separate entity ? J
Am Acad Dermatol 1989; 20: 338-41.
5. Roth MM. Pregnancy dermatoses: diagnosis, management,
and controversies. Am J Clin Dermatol.2011; 12:25-41.
6. Ott F, Krakowski A, Tur E , Lipitz R, Weisman Y , Brenner
S. Impetigo herpetiformis with lowered serum level of vitamin D and its
diminished intestinal absorption. Dermatologica 1982; 164: 360-5.
7. Lee SH, Hunt MJ, Barnetson RS. Pustular psoriasis of
pregnancy. Aust J Dermatol 1995; 36: 199-200.
8. Wolf R, Tartler U, Stege H, Megahed M, Ruzicka T. Impetigo
herpetiformis with hypoparathyroidism. J Eur Acad Dermatol Venereol 2005;
19: 743-6.
9. Oumeish OY, Farraj SE, Bataineh AS. Some aspects of impetigo
herpetiformis. Arch Dermatol 1982; 118: 103-5.
10. Macmillon AL, Champion RH. General pustular psoriasis
treated with dapsone. Br J Dermatol 1973; 88: 183-5.
11. Luewan S, Sirichotiyakul S, Tongsong T. Recurrent impetigo
herpetiformis successfully treated with methotrexate: a case report. J Obstet
Gynaecol Res. 2011; 37:661-663.
12. Hazarika D. Generalized pustular psoriasis of pregnancy
successfully treated with cyclosporine. Indian J Dermatol Venereol Leprol
2009; 75: 638.
13. Brightman L, Stefanato CM, Bhawan J, Phillips TJ. Third-trimester
impetigo herpetiformis treated with cyclosporine. J Am Acad Dermatol 2007;
56:S 62-4.
14. Patsatsi A, Theodoridis D, Vavilis D, Tzevelekis V,
Kyriakoua Kalabali Kiss D, Sotiriadis D. Cyclosporin in the management of
impetigo herpetiformis: a case report and review of the literature. Case
Rep Dermatol 2013 Jan-Apr; 5(1): 99-104
© 2014 Egyptian Dermatology Online Journal
|





